Women’s reproductive health encompasses a complex system and requires specialized medical care throughout all stages of life. Routine gynecology evaluations provide early detection for many underlying issues, helping women maintain their overall physical well-being. Navigating the various medical diagnoses can provide clarity for many patients.
What Is Gynecology?
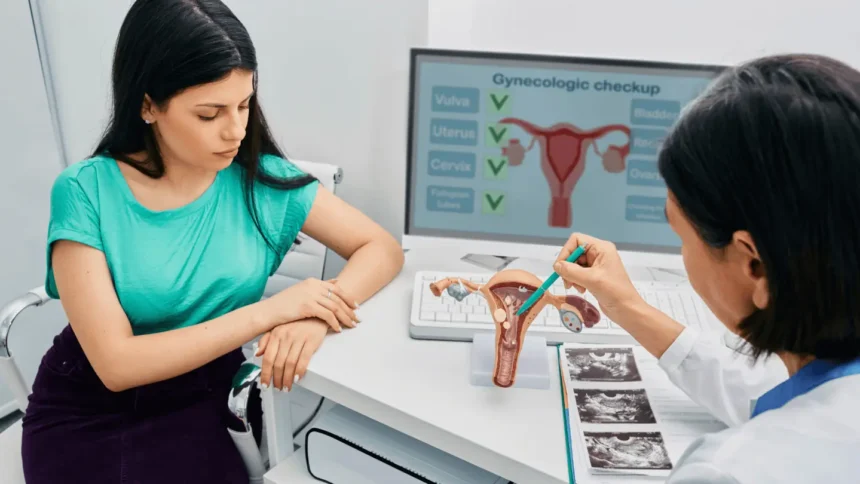
Gynecology functions as the branch of medicine focused specifically on the female reproductive system. Medical professionals in this field diagnose, treat, and monitor issues related to the uterus, ovaries, fallopian tubes, and vagina. Gynecologists provide preventative care, perform routine screenings like Pap smears, and address various reproductive health concerns. Many gynecologists also practice obstetrics, managing pregnancy and childbirth, though gynecology itself deals strictly with the reproductive system. Regular check-ups allow these doctors to track bodily changes over time, allowing them to provide early interventions and maintain detailed health histories.
What Conditions Fall Under It?
Gynecologists manage a wide array of medical issues. Endometriosis is a highly prevalent condition where tissue similar to the uterine lining grows outside the uterus. This abnormal growth causes significant pelvic pain and can lead to fertility challenges. Uterine fibroids represent another common diagnosis among women. These non-cancerous muscular tumors develop in or around the wall of the womb, frequently causing heavy menstrual bleeding and distinct pelvic pressure.
Polycystic ovary syndrome (PCOS) affects the body’s hormone levels, which often leads to irregular menstrual periods and metabolic changes. Medical professionals also evaluate and treat urinary incontinence, painful ovarian cysts, and abnormal uterine bleeding. On a more severe spectrum, specialists may diagnose various types of reproductive cancers, including cervical, uterine, and ovarian cancer. Each condition presents unique symptoms that require proper medical evaluation and a tailored diagnostic approach.
How Are They Treated?
Treatment plans vary widely and are based on the specific diagnosis, the severity of the symptoms, and the patient’s overall health profile. Doctors frequently prescribe medications as a primary, non-invasive intervention. Hormonal therapies, such as birth control pills or intrauterine devices (IUDs), can help regulate menstrual cycles and manage the painful symptoms associated with PCOS and endometriosis.
When conservative medical approaches fall short, targeted surgical interventions become necessary to restore health. Minimally invasive procedures allow surgeons to remove ovarian cysts or excise endometrial tissue using smaller incisions, which promotes much faster recovery times. For uterine fibroids, surgeons might extract the tumors while leaving the uterus intact. In more severe or life-threatening cases, surgeons might perform a hysterectomy to remove the uterus completely. Lifestyle modifications, targeted exercise regimens, and specific dietary adjustments may also play a significant role in managing chronic reproductive conditions and improving daily comfort.
Meet With a Gynecologist
Scheduling an appointment with a gynecologist serves as a proactive step toward maintaining long-term reproductive wellness. Beyond addressing immediate health concerns, these specialists can offer guidance on family planning, menopause management, and overall sexual health. Establishing a trusting relationship with a dedicated physician creates a safe environment that allows you to discuss highly sensitive health topics. Regular medical care gives you the knowledge and professional resources needed to navigate your reproductive health journey with clarity.