Chronic venous insufficiency is a condition that affects blood flow in the veins, most often in the legs, and can lead to ongoing discomfort, swelling, and skin changes over time. When left unaddressed, it may interfere with daily activities and increase the risk of further complications. Here is a closer look at the symptoms of venous reflux disease and management strategies:
Recognizing Warning Signs
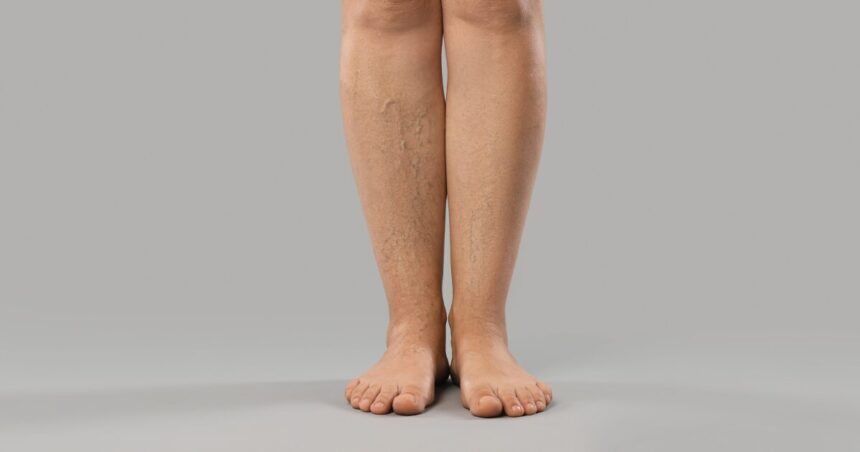
Patients with chronic venous insufficiency present specific physical signs that indicate abnormal blood flow in the legs. You should look out for the following warning signs:
- Swelling in the lower legs and ankles, especially after prolonged standing.
- Aching or tiredness in the legs that worsens throughout the day.
- New varicose veins that appear near the surface of the skin.
- Leathery skin changes or discoloration on the calves and ankles.
- Flaking or itching skin near the affected blood vessels.
Identifying these symptoms early can prevent severe complications like venous ulcers.
Identifying Contributing Factors
Several distinct factors cause venous valves to fail, leading to chronic venous insufficiency. Age plays a significant role in this process, as the wear and tear on the valves naturally increases over time. Family history also serves as a fundamental indicator, because genetics dictates the structural integrity of the vein walls.
Prolonged periods of standing or sitting restrict blood flow, and this inactivity places immense pressure on the lower body. Individuals who work at desks all day face a higher risk of developing venous reflux disease. Being overweight adds extra physical stress on the circulatory system, which forces the veins to work harder to transport blood upward. Previous blood clots, such as deep vein thrombosis, severely damage the valves inside the leg veins. Once a clot damages these structures, the veins lose their ability to maintain one-way blood flow.
Managing Symptoms
Physicians recommend several conservative approaches that target the underlying pressure in the affected veins. You can integrate the following habits into your daily routine:
- Wear prescription compression stockings to assist the veins in pushing blood upward.
- Elevate your legs above heart level multiple times a day to reduce swelling.
- Practice regular exercise to strengthen the calf muscles and improve circulation.
- Maintain a healthy body weight to decrease the overall pressure on the lower extremities.
- Avoid long periods of standing or sitting to keep the blood moving properly.
Implementing these lifestyle changes helps control the physical discomfort associated with the condition.
Knowing When Care Matters
Managing venous reflux disease requires consistent monitoring because the condition does not resolve on its own. Regular check-ups with a vascular specialist allow patients to track changes in their leg health. If conservative measures fail to control the swelling and pain, the specialist will recommend medical procedures to close the damaged veins.
Vascular specialists use ultrasound technology to observe the blood flow and locate the exact areas of valve failure. This diagnostic tool provides accurate data, and it helps the physician develop a precise treatment strategy. Following a structured care plan remains fundamental to preventing permanent tissue damage and open sores.
Schedule Your Chronic Venous Insufficiency Consultation
Chronic venous insufficiency alters normal leg circulation and causes symptoms such as swelling, aching, and skin discoloration. Recognizing the contributing factors and implementing conservative management strategies form the foundation of effective control. Patients must prioritize their vascular health and monitor their condition closely in collaboration with a trained medical professional. For signs of venous reflux disease, contact a qualified vascular specialist near you to schedule your appointment today.